Reimagining Care Delivery Through Intelligent Tools and Patient-First Design
Healthcare is in the midst of a radical shift. As traditional, fee-for-service models give way to value-based care, providers are under mounting pressure to deliver better outcomes at lower costs—without sacrificing the patient experience.
But how do you manage rising complexity, coordinate across fragmented systems, and keep patients engaged every step of the way? That’s where accountable care technology comes in.
More than just a buzzword, it represents a new generation of digital tools and platforms built specifically to support the goals of accountable care organizations (ACOs). In an era where data overload, clinician burnout, and health disparities threaten progress, this technology offers a path forward. It’s not about adding more to providers’ plates—it’s about making smarter, more connected care possible. If you’re ready to see how emerging tech is reshaping the future of accountable care, you’re in the right place.
The Power of Emerging Tech in Accountable Care
At its core, accountable care is about aligning incentives so providers focus on outcomes, not just services rendered. But that mission is nearly impossible without the right tools, and that’s where accountable care technology steps in.
These technologies function as the essential connectors within the healthcare ecosystem, integrating data, teams, and workflows across the care continuum. By centralizing information and making it accessible and actionable, accountable care technology empowers providers to deliver coordinated, cost-effective, and patient-centered care that improves outcomes while enhancing satisfaction.
1. Interoperability: Breaking Down Data Silos
One of the biggest headaches in accountable care is fragmented data. When systems can’t communicate, providers end up making decisions based on incomplete information. That’s where accountable care technology steps in.
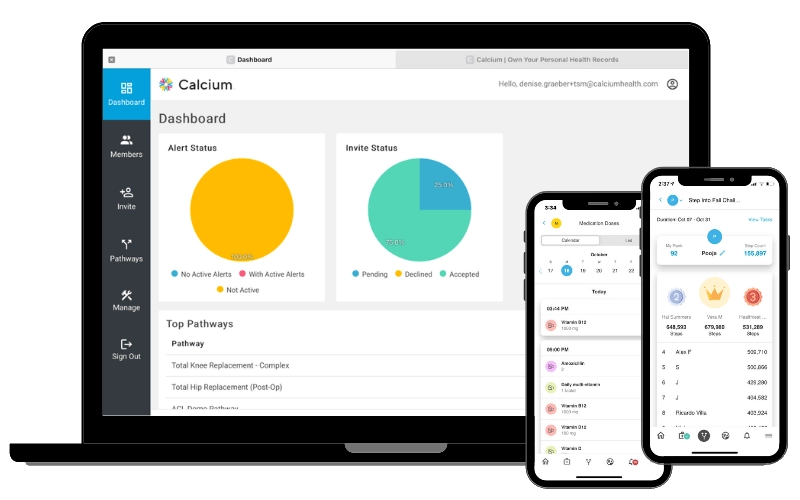
Modern platforms like Calcium now focus on interoperability—connecting EHRs, labs, pharmacies, and patient-reported data into one unified ecosystem. This real-time, 360° view of the patient empowers care teams to make faster, smarter, and more proactive decisions (Balio et al., 2019).
And as highlighted in the literature on federated learning, these technologies can even share predictive insights without compromising patient privacy (Nguyen et al., 2021). That’s a game-changer for data sharing across networks.
2. Telemedicine as a Cornerstone of Continuity
Telemedicine isn’t just a COVID-era convenience—it’s become a backbone of accountable care technology. Virtual visits help maintain continuous contact between patients and their care teams, especially for those managing chronic illnesses or behavioral health conditions.
Plus, telehealth:
- Reduces transportation and scheduling barriers
- Enhances patient engagement with more flexible touchpoints
- Supports collaborative care by bringing in specialists without referrals or wait times
- Connects patients with mobility issues, transportation barriers, or busy schedules
For accountable care organizations (ACOs), this translates into fewer missed appointments and better adherence to care plans (Modi et al., 2019).
3. Predictive Analytics and Risk Stratification
What if you could identify at-risk patients before they show up in the ER?
That’s the promise of AI-driven accountable care technology. With predictive analytics and risk stratification, ACOs can zero in on high-risk populations and intervene early—often with virtual check-ins, nurse outreach, or social services support.
Here are a few key ways eHealth supports population health:
- AI-driven alerts flag patients who are trending toward adverse outcomes
- Digital care plans automate follow-up and monitoring tasks
- Wearables and remote monitoring tools feed real-time data back into clinical systems
According to the study on federated learning in healthcare, AI models trained across decentralized datasets can enhance these capabilities while respecting patient confidentiality—a critical feature for health systems and regulators (Nguyen et al., 2021).
4. Enhancing the Patient Experience
Accountable care can’t succeed without patients on board. That’s where user-friendly, patient-facing tools come in. Whether it’s a mobile health app or a personalized health portal, these technologies give patients more control, transparency, and connection to their care.
And let’s be honest—when was the last time you remembered a doctor’s advice word-for-word after leaving the clinic?
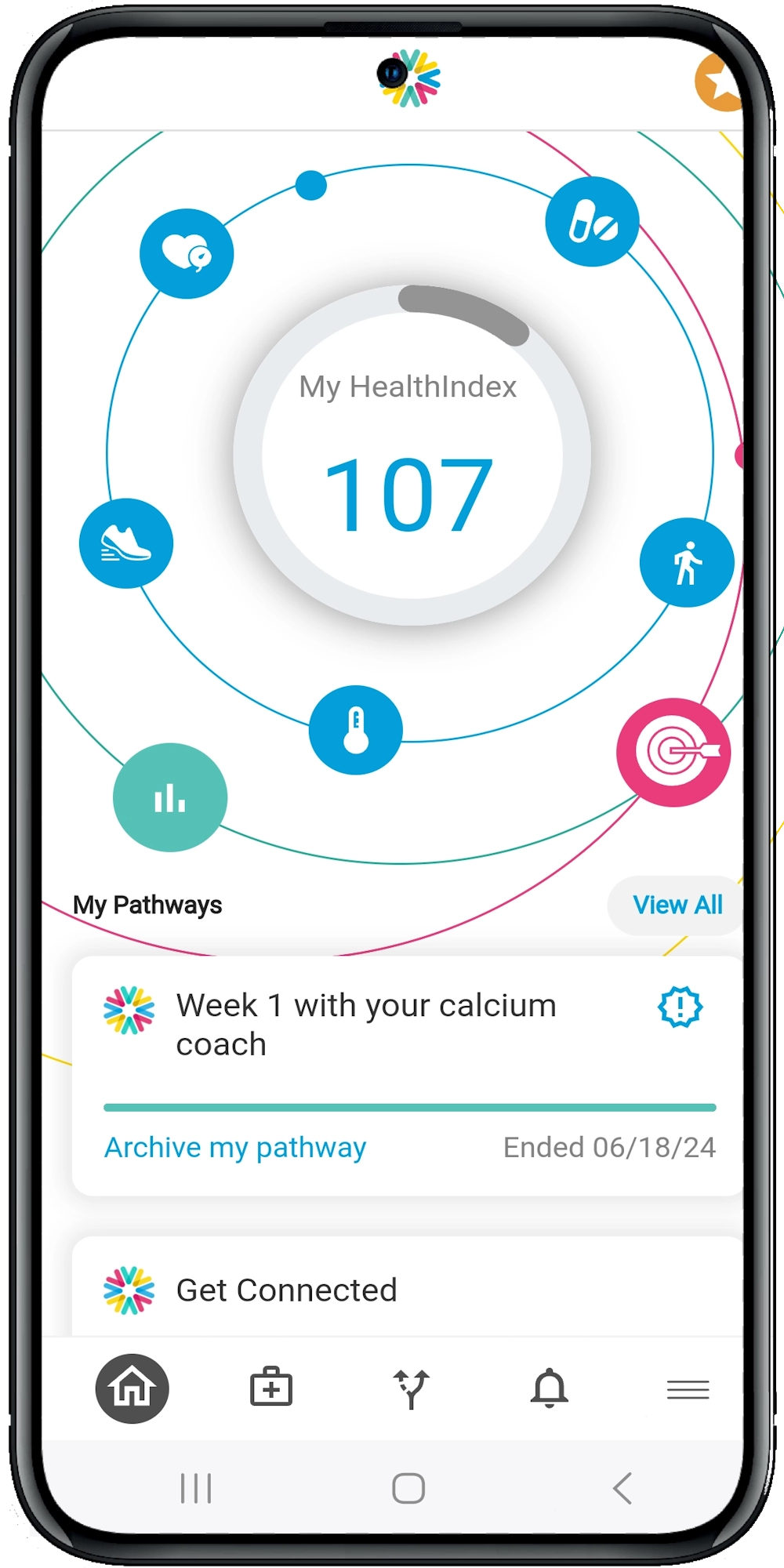
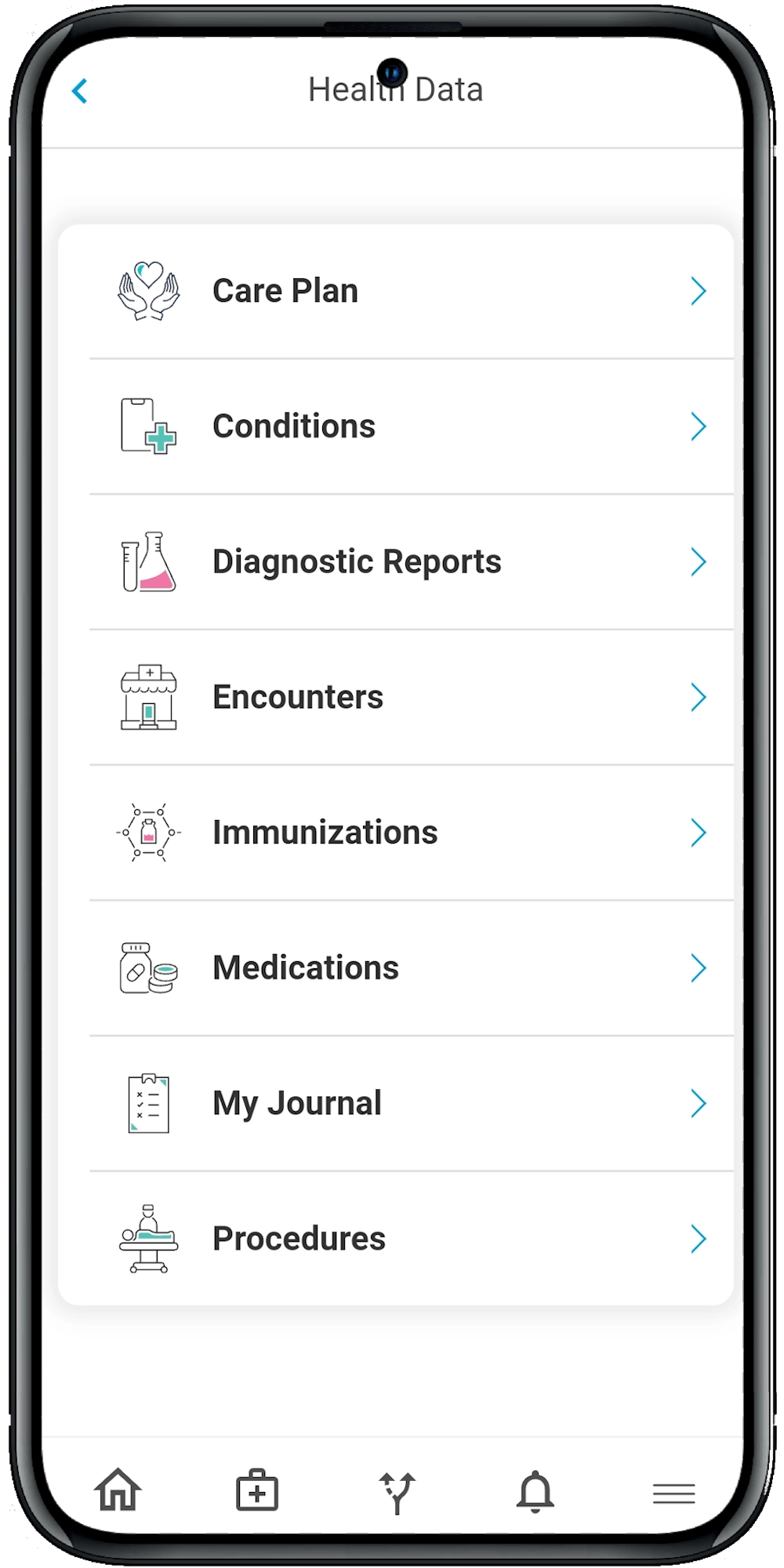
Calcium’s Super App empowers patients with features like medication management, health journaling, access to personalized health pathways and secure messaging with care teams. Such platforms help keep patients informed and involved in their own health journey (Mohd Fadhil et al., 2022).
5. Tackling Social Determinants of Health (SDOH)
No digital strategy is complete without addressing what really drives health outcomes: where and how people live.
eHealth tools help providers screen for and respond to SDOH factors like food insecurity, housing instability, and transportation access. Some platforms even embed community resource referrals into the care workflow. Imagine finishing a telehealth visit and immediately being connected to a local food bank or transportation service. That’s the future of accountable care—and it’s already happening.
6. Behavioral Health Integration Through Digital Tools
Mental health isn’t a side dish—it’s a core part of whole-person care. Accountable care technology is bridging the gap between physical and behavioral health, allowing ACOs to integrate services in a seamless, patient-centered way (Modi et al., 2019).
Tools that support this integration include:
- Digital mental health assessments embedded into primary care visits
- Secure video counseling within patient apps
- Real-time symptom tracking via mood journals or wearable sensors
By embedding behavioral health into everyday care, providers can better manage conditions like depression, anxiety, and substance use—often reducing ER visits and improving adherence to medical treatment.
Calcium enhances behavioral health integration through its platform, offering tools that support mental health assessments and secure communication between patients and providers.
7. Outcome Measurement and Reporting
You can’t improve what you don’t measure. The best accountable care technology doesn’t just support care delivery—it tracks the outcomes that matter. We’re talking about:
- Quality metrics (HEDIS, STAR, etc.)
- Patient-reported outcomes (PROMs)
- Population-level insights
Real-time dashboards help care teams adjust care plans on the fly, ensuring that interventions stay effective and cost-efficient. This isn’t just about compliance—it’s about continuous improvement (Balio et al., 2019).
And when data flows automatically from platform to payer, ACOs spend less time on manual reporting and more time on actual care.
Future Trends: What’s Next for eHealth in Accountable Care?
The digital health space is evolving rapidly. Here are a few emerging trends to watch:
- Federated Learning and Privacy-Preserving AI. Instead of sharing raw patient data, federated learning allows systems to collaborate on training AI models without compromising privacy. This approach supports better predictive analytics across diverse populations while protecting patient confidentiality.
- Consumer-Grade User Experience (UX). Patients now expect healthcare apps to work like the best apps on their phones—simple, intuitive, and responsive. The more ACOs invest in UX, the higher their engagement rates will climb.
- Integrated Care Pathways. Platforms that guide patients through complex treatment journeys with digital “pathways” are becoming increasingly popular. These tools provide tailored education, appointment reminders, and ongoing check-ins—all in one experience. Calcium’s AI Studio allows providers to design and personalize automated pathways, guiding patients through their health journeys effectively
- Digital Therapeutics and RPM (Remote Patient Monitoring). From digital CBT for anxiety to glucose monitoring for diabetes, therapeutic apps are starting to complement or even replace traditional medications.
The Wrap
As the healthcare landscape evolves, accountable care technology is no longer optional—it’s essential. From integrating behavioral health and remote monitoring to empowering patients through personalized engagement, today’s digital tools are redefining what’s possible in value-based care.
But not all platforms are created equal. The most effective solutions go beyond tech—they support the people behind the care: the clinicians, care coordinators, and patients working toward better outcomes together.
At Calcium, we’ve built a digital health platform that brings these innovations to life. With customizable care pathways, real-time analytics, and seamless interoperability, we help providers deliver smarter, more accountable care—every step of the way.
Reference
Balio, C. P., Apathy, N. C., & Danek, R. L. (2019). Health Information Technology and Accountable Care Organizations: A Systematic Review and Future Directions. EGEMS (Washington, DC), 7(1), 24. https://doi.org/10.5334/egems.261
Modi, P. K., Kaufman, S. R., Portney, D. S., Ryan, A. M., Hollenbeck, B. K., & Ellimoottil, C. (2019). Telemedicine utilization by providers in accountable care organizations. MHealth, 5, 10–10. https://doi.org/10.21037/mhealth.2019.03.02
Nguyen, D. C., Pham, Q.-V., Pathirana, P. N., Ding, M., Seneviratne, A., Lin, Z., Dobre, O. A., & Hwang, W.-J. (2021). Federated Learning for Smart Healthcare: A Survey. ArXiv:2111.08834 [Cs, Eess]. https://arxiv.org/abs/2111.08834
Mohd Fadhil, N. F., Teoh, S., & Wickramasinghe, N. (2022). Leveraging value-based care principles in developing eHealth systems: A teaching case. Journal of Information Technology Teaching Cases, 204388692110632. https://doi.org/10.1177/20438869211063219