Enabling Seamless Care Delivery Through Smarter Health Technology
The U.S. healthcare system is in the middle of a high-stakes transformation — shifting from volume to value, from isolated encounters to connected care. At the heart of this change is the accountable care network, a model that demands providers work together to deliver better outcomes at lower costs. But most networks are still cobbling together fragmented systems, outdated workflows, and one-size-fits-all tools. And patients? They’re often stuck navigating the chaos alone.
To succeed in this new era, ACNs need more than cooperation — they need connection. That means breaking down data silos, integrating post-acute partners, engaging patients daily, and supporting every corner of the care team with smart, real-time tools. This isn’t just a technology challenge — it’s a human one. If we’re serious about value-based care, we have to get serious about the digital infrastructure that makes it possible. Let’s talk about how to build it.
What Makes an Accountable Care Network So Challenging?
If you’re part of an accountable care network (ACN), then you already know — it’s no walk in the park. At its core, an ACN brings together hospitals, primary care practices, specialists, post-acute providers, and community-based organizations to deliver coordinated care. Its goal is to provide better outcomes at a lower cost.
But here’s the catch: Most of these providers operate in different systems, speak different “data languages,” and have vastly different resources. It’s like trying to conduct an orchestra when half the musicians are playing from different sheet music — and some don’t even have instruments yet.
So what’s standing in the way of seamless care? Let’s break down the key roadblocks that keep ACNs from reaching their full potential.
1. Unified Data Views that Eliminate Silos
Data silos might be the most frustrating issue ACNs face. Each provider in the network often uses a different electronic health record (EHR) system. Data doesn’t move easily. Even when it does, it’s incomplete or outdated.
A recent study in The American Journal of Managed Care found that while ACO hospitals were more likely to participate in health information exchanges, there was still huge variability in IT capabilities across organizations. That means some providers are data-rich and others are flying blind (Walker et al., 2016).
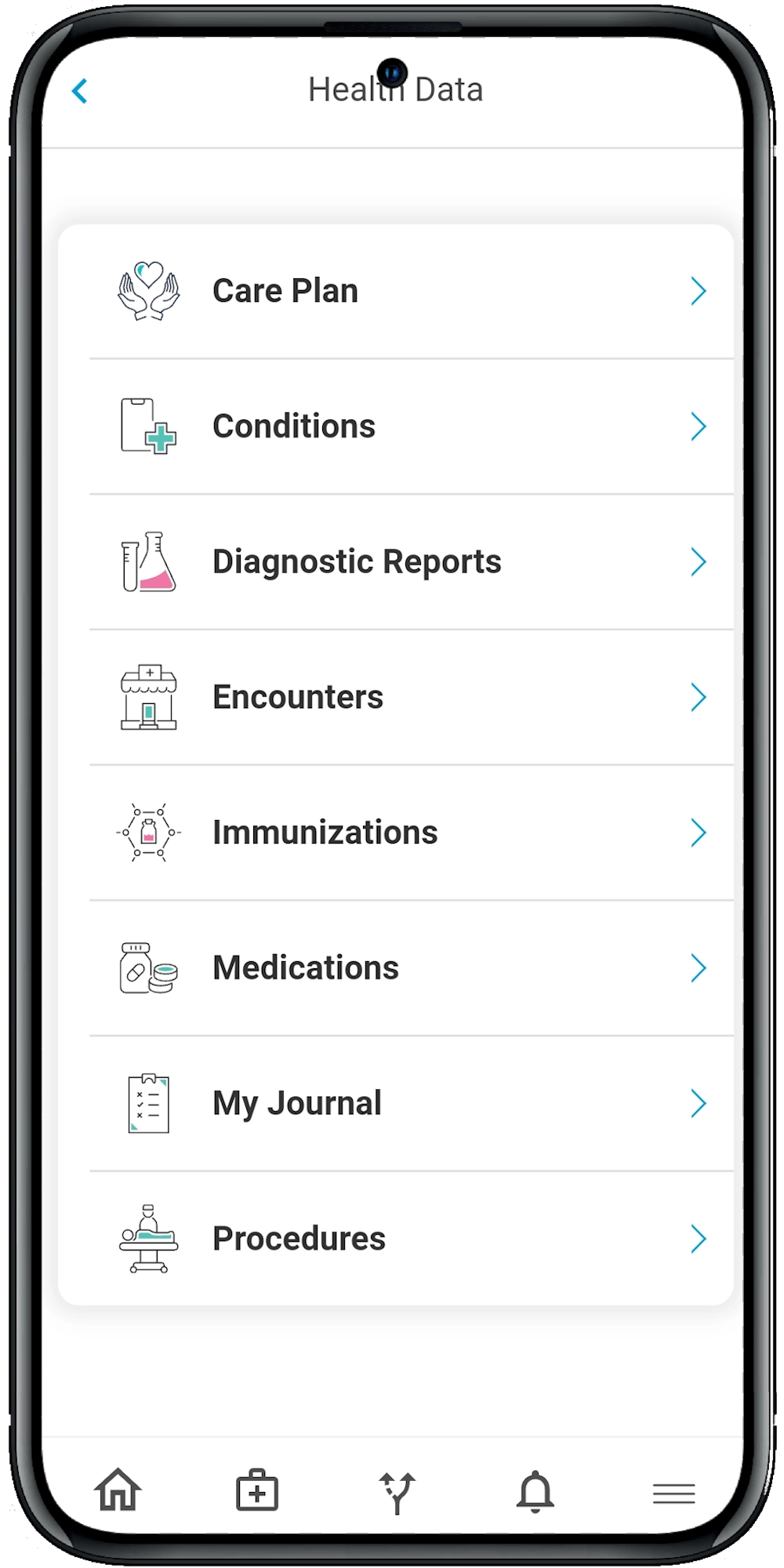
Without a unified data view, it’s hard to spot trends, track risk, or manage care effectively. Smart integration platforms and digital care pathways can consolidate information from EHRs, wearables, apps, and even patient self-reports into one actionable view.
2. Seamless Integration with Post-Acute Care
Discharging a patient to a skilled nursing facility (SNF) shouldn’t feel like sending them into a black hole — but too often, it does. Many accountable care networks still struggle to align with SNFs, rehab centers, and other post-acute providers. These groups might not have the same tech tools or quality reporting systems in place.
A study in the Journal of the American Geriatrics Society showed how one ACO worked around this by building a preferred SNF network. They selected facilities with higher CMS star ratings, quicker physician response times, and stronger clinical oversight. But even then, keeping those connections active took serious work (Lage et al., 2015).
Smart data tools help here by offering real-time monitoring, medication tracking, and compliance alerts even after discharge. With platforms like Calcium, SNFs can share updates, providers can intervene early, and patients avoid unnecessary ER visits.
3. Bundled Care Opportunities
Bundled care models are supposed to streamline how we manage common conditions or procedures — like knee replacements, heart failure, or childbirth. But knowing which conditions to bundle (and how to track them) is still a mystery for many ACNs.
Smart analytics can identify these patterns early, helping ACNs optimize care bundles.
One preprint study used EMR data and machine learning to identify common condition clusters that naturally share workflows—from prostate issues to complex pregnancies. The takeaway? There are real opportunities for bundled care hiding in your data. You just need the right tools to surface them (Chen et al., 2017).
Using digital care pathways powered by AI, ACNs can surface these patterns, map patient journeys, and create shared protocols to ensure each provider is on the same page.
4. Scalable Solutions for Safety-Net Providers
Community health centers and federally qualified health centers (FQHCs) are critical to reaching underserved populations. But they’ve often been left out of the accountable care movement. Why? Because they usually don’t have the IT infrastructure or funding to join in.
But that’s changing.
In a national survey, nearly one-third of ACOs now include community health centers as official partners. These groups bring unmatched expertise in primary care and social determinants of health. Still, integration isn’t easy — especially when those centers lack access to advanced IT or real-time data tools (Lewis et al., 2014).
Scalable digital tools — ones that don’t require major IT investments — can help safety-net providers participate more fully by offering access to care pathways, dashboards, and communication tools used across the network..
5. Persistent Patient Engagement Beyond the Clinic
Even the best care plan won’t work if the patient doesn’t follow it. One of the biggest challenges for any accountable care network is patient adherence.
Think about it: Patients leave the clinic with a list of meds, dietary changes, therapy sessions, and follow-up appointments — and then real life hits. Work, stress, financial strain, or just forgetfulness all get in the way.
To close that loop, ACNs need to engage patients beyond the clinic.
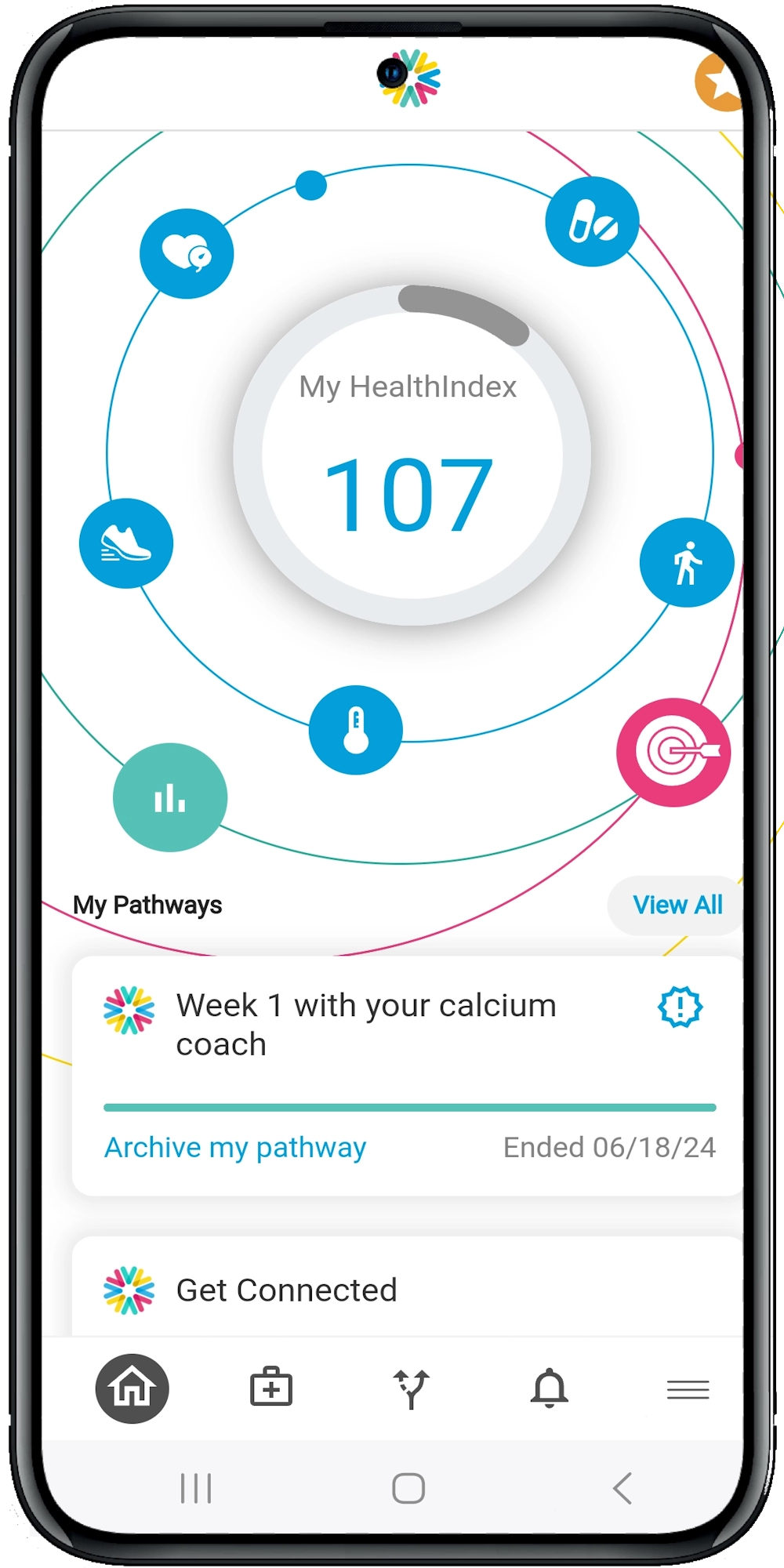
With smart apps like Calcium’s Super App, patients get daily nudges — reminders to take meds, record symptoms, log meals, or just check in. The app also delivers motivational messages, educational videos, and even allows family members to participate in the care plan. It’s not just about keeping patients informed. It’s about keeping them connected.
6. Real-Time Visibility into Population Health
Most ACNs are flying blind when it comes to real-time population health. Sure, you can pull reports monthly or quarterly, but by then the damage is done. Patients have already ended up in the ER or missed key milestones.
To stay ahead, you need tools that flag risk early — not after the fact.
Digital health platforms provide dashboards that track key health indicators in real time. Imagine getting an alert when a diabetic patient’s glucose logs are trending upward, or when a heart failure patient hasn’t logged any weight data in three days. These early signals let care teams reach out, adjust meds, and avoid costly complications.
7. Collaborative Platforms that Power Team-Based Care
In an ideal accountable care network, the patient flows smoothly between providers, and everyone stays in sync. But in reality, PCPs, specialists, nurses, and case managers are often working in parallel — not together. A major reason? Lack of shared tools.
Without a central platform to assign tasks, monitor compliance, and communicate across teams, care gets fragmented. Duplicate tests get ordered. Follow-ups get missed. And the patient ends up frustrated.
Team-based digital care tools help address this challenge by enabling everyone — from doctors to dietitians — to access the same care plan, communicate securely, and track patient progress in one centralized platform. It’s like giving every player on the field the same playbook, all in real time.
The Wrap
Accountable care networks were designed to bring healthcare into a more connected, patient-centered future — but without the right digital tools, even the best intentions fall short. Each of these roadblocks — from siloed data to disengaged patients — can be overcome with the right digital foundation. Smart data platforms like Calcium aren’t just helpful add-ons; they’re essential infrastructure for making value-based care actually work.
From uniting fragmented data to engaging patients with daily health guidance, Calcium empowers ACNs to coordinate more effectively, respond faster, and deliver measurable results. It’s how you move from checking boxes to truly transforming care. If your organization is ready to break down silos, boost collaboration, and take ownership of better outcomes, now’s the time to explore what’s possible.
Reference
- Chen, Y., Kho, A. N., Liebovitz, D., Ivory, C., Osmundson, S., Bian, J., & Malin, B. A. (2017). Learning Bundled Care Opportunities from Electronic Medical Records. ArXiv.org. https://arxiv.org/abs/1706.00487
- Lewis, V. A., Colla, C. H., Schoenherr, K. E., Shortell, S. M., & Fisher, E. S. (2014). Innovation in the Safety Net: Integrating Community Health Centers Through Accountable Care. Journal of General Internal Medicine, 29(11), 1484–1490. https://doi.org/10.1007/s11606-014-2911-0
- Walker, D. M., Mora, A. M., & Scheck McAlearney, A. (2016). Accountable care organization hospitals differ in health IT capabilities. The American Journal of Managed Care, 22(12), 802–807. https://pubmed.ncbi.nlm.nih.gov/27982667/
- Lage, D. E., Rusinak, D., Carr, D., Grabowski, D. C., & Ackerly, D. C. (2015). Creating a Network of High-Quality Skilled Nursing Facilities: Preliminary Data on the Postacute Care Quality Improvement Experiences of an Accountable Care Organization. Journal of the American Geriatrics Society, 63(4), 804–808. https://doi.org/10.1111/jgs.13351