Smart Tools for Scaling Patient-Centerd Surgery Without Adding Overhead
Running a successful Ambulatory Surgery Center (ASC) in today’s healthcare landscape is no small feat. Between tighter margins, increasing patient demand, and complex regulatory requirements, many ASC leaders feel like they’re juggling scalpels while sprinting. Yet the real differentiator for long-term growth isn’t just surgical volume—it’s how smart your technology is.
In an industry shifting rapidly toward value-based care, efficiency and experience matter more than ever.
So why are so many ASCs still relying on outdated systems or fragmented tools? If you’re serious about expanding services without sacrificing quality, you need more than good intentions—you need a digital foundation that’s built to scale. In this post, we’re exploring the essential health tech stack every forward-thinking ASC should consider.
Whether you’re managing one center or preparing to open three more, the right tech strategy could be the difference between sustainable growth and operational burnout. Let’s take a closer look at what’s required.
What Is a Health Tech Stack for ASCs?
Think of your health tech stack like the surgical tray in an operating room—every tool should be clean, connected, and easy to reach. In Ambulatory Surgery Centers (ASCs), your tech stack is the combination of digital tools you use to run operations, deliver care, and grow efficiently. When it’s well-designed, your staff saves time, your patients stay engaged, and your billing system doesn’t become a bottleneck.
But if your tools don’t talk to each other, you’re essentially operating in the dark. And that’s a huge risk, especially when you’re scaling.
A strong tech stack allows ASCs to evolve from paper processes and disconnected systems into streamlined engines of value-based care. It helps you deliver better outcomes at a lower cost while meeting growing patient demand.
7 Tech Challenges That Stall ASC Growth
Before diving into the must-have components, let’s acknowledge the major roadblocks that often hold ASCs back. Based on extensive studies and national surveys, these are the most common tech pain points for expanding ASC programs:
- Low Adoption of EHRs and HIT
Nearly half of ASCs still don’t use EHRs, according to a Wisconsin survey. And over one-third have no access to even basic EHR features. That’s a glaring vulnerability when patient transitions, documentation, and billing all rely on data continuity. - Fragmented and Non-Interoperable Systems
Health IT systems often fail to communicate across care settings. This disconnect puts patients at risk during handoffs and leads to care delays, duplicate tests, and preventable errors. - High Implementation Costs
For smaller ASCs, investing in robust technology systems feels out of reach. Initial setup and staff training can cost tens of thousands per provider, which makes ROI a lingering concern. - Manual Workflows and Inefficiencies
From pre-op assessments to post-op instructions, many ASCs still depend on paper forms, faxes, and in-person follow-ups. These delays reduce provider productivity and make scaling more difficult. - Regulatory Pressures and Compliance Gaps
ASCs face evolving requirements from CMS and the FDA. For instance, even cables connecting medical devices to IT systems can be classified as “medical devices,” bringing new compliance responsibilities. - Poor Patient Engagement Tools
In today’s mobile-first world, patients expect reminders, digital check-ins, and personalised instructions. Many ASCs don’t have the platforms to meet those expectations, which can hurt satisfaction scores and follow-up compliance. - Unstable Reimbursement for Digital Services
While telehealth has proven value in ASCs, reimbursement models haven’t caught up. Without clear billing paths, many centers hesitate to invest in virtual care infrastructure.
These challenges aren’t just inconvenient—they directly limit your ability to grow. But with the right health tech stack, you can overcome each one.
What Should Be in Your ASC Health Tech Stack?
Building the right foundation starts with identifying the tech categories that make your ASC faster, safer, and more scalable. Here are the essential layers your digital stack should include.
1. ASC-Optimised EHR & Clinical Documentation Tools
Generic EHRs often fail to meet the unique needs of outpatient surgical centers. You need a system designed for high-volume, short-stay procedures, with built-in support for anaesthesia documentation, pre-op screening, and surgical scheduling.
Look for:
- Customizable templates specific to ASC workflows
- Real-time charting and order entry
- One-click access to past surgical histories
- Built-in coding and billing support
The goal? No more flipping between screens or waiting for chart updates—just smooth, real-time clinical coordination.
2. Smart Scheduling and Practice Management
A fully booked schedule doesn’t mean an efficient one. Smart scheduling tools allow you to automate case bookings, avoid resource conflicts, and balance high-revenue procedures throughout the week.
Key features to look for:
- Integration with EHR, billing, and staff rosters
- Block scheduling rules for ORs
- Text/email appointment reminders
- Waitlist management to fill late cancellations
Every open slot is a missed opportunity. Smart scheduling helps you maximise daily case volume without burning out your staff.
3. Telehealth for Pre- and Post-Operative Care
Why have patients drive across town for a five-minute follow-up? Research from MUSC shows that replacing manual steps with telehealth improves ASC efficiency and expands provider capacity.
Here’s where telehealth shines in ASCs:
- Pre-op consults for low-risk patients
- Post-op wound checks and pain assessments
- Medication reconciliations
- Patient education and informed consent
It’s not about replacing surgeons with screens—it’s about using tech to free up OR time and streamline repetitive tasks.
4. Patient Engagement Platforms
Your patients use smartphones for everything else—why not for their surgery journey? Modern patient engagement tools reduce no-shows, improve compliance, and keep patients in the loop.
The best platforms offer:
- Mobile-friendly portals for check-ins and forms
- Automated reminders for pre-op fasting or medication holds
- Real-time messaging with care teams
- Multilingual educational materials
A well-informed patient is a safer patient. And when they feel supported, your satisfaction scores go up.
5. Revenue Cycle Management & Billing Tools
Billing errors and delays can kill your cash flow. And expanding ASCs often struggle with growing payer mixes, out-of-network claims, and prior authorisations.
A good tech stack will help you:
- Automate eligibility checks and authorisation workflows
- Generate clean claims with proper surgical codes
- Track denials and underpayments in real time
- Provide transparent cost estimates to patients
With reimbursement cuts and narrow networks on the rise, your revenue cycle tools must be as precise as your surgical instruments.
6. Real-Time Data Analytics and Reporting
You can’t improve what you don’t measure. Analytics platforms allow ASC leaders to monitor clinical outcomes, operational KPIs, and financial performance all in one place.
Look for:
- Dashboards showing case volume, turnover time, cancellations
- Benchmarking against similar centers
- Quality metrics tied to value-based contracts
- Predictive insights to prevent readmissions or cancellations
Analytics isn’t just for the C-suite. Giving frontline staff access to their metrics helps drive continuous improvement.
7. Security and Compliance Infrastructure
As your digital footprint grows, so do cybersecurity risks. You need layered defences and role-based access to keep patient data safe and regulators satisfied.
Security essentials:
- HIPAA-compliant cloud infrastructure
- Multi-factor authentication for all users
- Encrypted device integration (especially for telehealth)
- Real-time breach alerts and audit trails
Don’t forget: the FDA now regulates even some device-IT cables. A secure setup protects you from more than just hackers—it guards against regulatory blowback.
Why It All Matters
Expanding an ASC isn’t just about more procedures—it’s about doing more with less. Technology should reduce burdens, not add new ones. But it only works when your tools are interoperable, customizable, and designed for your workflows.
A strong tech stack can help you:
- Scale without hiring an army of new staff
- Improve throughput without compromising quality
- Engage patients from referral to recovery
- Stay ahead of regulatory and reimbursement shifts
In a space as fast-paced and competitive as ambulatory surgery, relying on outdated tech is like using a flip phone to manage a trauma case—it simply doesn’t keep up. Building a smart, scalable digital foundation isn’t just a nice-to-have anymore—it’s essential for sustainable growth, better patient outcomes, and financial resilience.
Whether you’re aiming to reduce cancellations, boost staff efficiency, or stay compliant as your center expands, the right technology stack can turn those goals into reality.
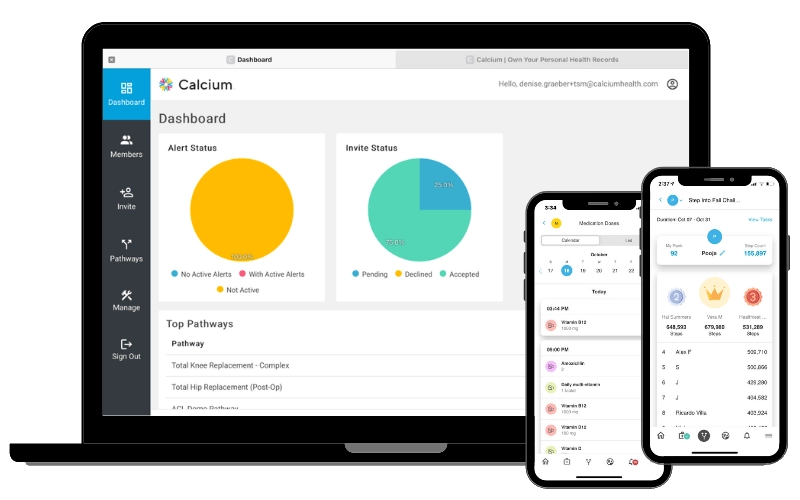
That’s where the Calcium digital health platform comes in. Purpose-built for modern ASCs, Calcium offers integrated tools for care coordination, patient engagement, analytics and remote care—all in one easy-to-navigate system.
The right technology stack isn’t a luxury—it’s a survival kit for modern ASCs.
References
- Pai, S.-L., Ladlie, B., Locke, K., & Getting, R. G. (2024). Patient-Centered Care for Ambulatory Surgery. International Anesthesiology Clinics, 63(1), 14–22. https://doi.org/10.1097/aia.0000000000000461
- Robertson, D. C., & Lerner, J. C. (2009). Top Technology Issues for Ambulatory Care Facilities This Year and Beyond. Journal of Ambulatory Care Management, 32(4), 303–319. https://doi.org/10.1097/jac.0b013e3181ba6f86
- Allison, K. (2021). Assessing Transformation of Optimizing Ambulatory Surgery Center Services with Telehealth. MUSC Theses and Dissertations. https://medica-musc.researchcommons.org/theses/648/
- Establishing and Managing an Ambulatory Surgery Center:… : International Anesthesiology Clinics. (2025). LWW. https://doi.org/10.1097/AIA.0000000000000465
- Wiggins, C., Peterson, T., & Moss, C. (2015). Ambulatory surgery centers׳ use of Health Information Technology. Health Policy and Technology, 4(2), 100–106. https://doi.org/10.1016/j.hlpt.2015.02.006
- Manchikanti, L., Parr, A. T., Singh, V., & Fellows, B. (2011). Ambulatory surgery centers and interventional techniques: A look at long-term survival. Pain Physician, 14(2), E177. https://www.painphysicianjournal.com/current/pdf?article=MTQ1MQ%3D%3D&journal=60
- Health information technology for ambulatory care in health systems. (2020). The American Journal of Managed Care, 26(1), 32–38. https://doi.org/10.37765/ajmc.2020.42143